Last month, I said I would unpack what the Lancet Commission means for Malaysia in my next column. I will in January. This month, I want to make a detour. If we are serious about cancer care that cares, there is one quiet thing we do not talk about enough. I found myself thinking about it during my visiting fellowship at the National Cancer Center Korea (NCC Korea).
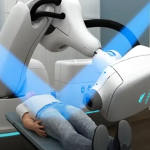
As I walked into the centre, I felt a familiar mix of awe and humility. In places like this, “advanced cancer care” is not merely a slogan. Among the awe-inspiring services at NCC Korea, one of the grandest, most impressive and frankly unignorable was proton therapy, a specialised form of radiotherapy used for selected cancers. Unlike conventional radiotherapy, where radiation continues travelling through the body, a proton beam can be planned to deliver its punch at the tumour and then fade quickly, reducing unnecessary radiation beyond it. So yes, the wow was the proton beam and the cyclotron behind it (the machine that generates the beam), the kind of infrastructure that can cost hundreds of millions of US dollars to set up. But the deeper lesson was not the machine.
It was how the state-of-the-art institution was run. Decisions were made, checked, documented and handed over so that the next clinician, the next team, the next service does not start from zero. At the heart of this story is a simple point… A proton beam does not deliver good care on its own. A system does. Proton therapy grabs our attention because it looks like the future for the Malaysian healthcare. But the more important future is invisible. It is a record that follows the patient so that clinical care does not reset at every doorway. That record can live in the system (electronic medical record [EMR]), and it can also be held by the patient, so that they are not forced to repeat their stories, or carry papers and screenshots between departments, or physicians chasing paper records that go missing or get held up elsewhere. While this “information continuity” may not seem to be the headline part of cancer care, it is what makes the patient’s journey feel smooth, respectful and safe.
Back home in Malaysia, the one question that kept tugging at me was, “Are we building the information threads that make cancer care truly people-centred?”
This is where Malaysia’s current direction matters. We are hearing more clearly now about “One Person, One Record”, a Malaysian Ministry of Health’s effort to strengthen and connect EMR across the health system so information can be accessed more reliably where it is needed. If it is done well, it should reduce duplication, delays, and the safety risks associated with fragmented care. At the same time, there is also the patient-facing side of this same ambition, what they can see, hold, and use. A recent conversation with Dr Mahesh Appanan from the Digital Health Division of Ministry of Health Malaysia made me unexpectedly optimistic. He told me that MySejahtera has been integrated with systems such as pharmacy, dental, and screening platforms, aligned with a broader direction towards “One Person, One Record”. In plain language, this means some Malaysians can already view parts of their health information digitally.
For cancer, this matters because the patient’s journey is rarely confined to one place. People move between clinics, hospitals, imaging centres, pharmacies, and sometimes between public and private care. When information does not follow the person, the system quietly shifts the burden back to the patient to bring the documents, remember the dates, repeat the story and explain what happened elsewhere.
We also need to be honest about where Malaysia is today. Our digital landscape is uneven. Clinical care is still paper-heavy, EMRs are not universal, and even when systems exist, they do not always speak to one another. This is also where patient-held records matter, not as a tech trend but as a practical tool that can reduce burden while the bigger system integration is still being built.
Digital health transformation also triggers questions about privacy and cybersecurity, and about who controls the system, who can access the data and what happens when something goes wrong. In a cancer journey, where vulnerability is high and the stakes are personal, trust is not optional. So, what would it take for national records and patient-held records to earn trust in Malaysian cancer care?
It starts with being clear. People should not need to go to extra lengths to find out what medical information exists, where it sits, and what it is useful for. If digital records are meant to reduce burden, the benefits have to show up in every clinical encounter. It also requires safeguards people can see and understand, meaningful privacy protections, accountability when things go wrong, and genuine consent. None of this works without the health system getting it right. Training, workflows, and change management matter as much as the platform. Most importantly, patients and clinicians have to be treated as partners, with a real voice in how a lifelong record is designed, explained, protected and improved.
Standing in one of the most sophisticated cancer centres in the world can make our health system feel “behind.” But my strongest takeaway is much more hopeful. Malaysia is already making progress. The next step is not only about scaling up. It is about earning trust deliberately and transparently, and with humility. Because in cancer care, even a state-of-the-art technology still depends on something basic, a medical record that follows the patient safely, accurately and continuously, in a system that people can trust.